Procedures
___________________________________________________________________________________
Root Canal Treatment
What is Root Canal Therapy?
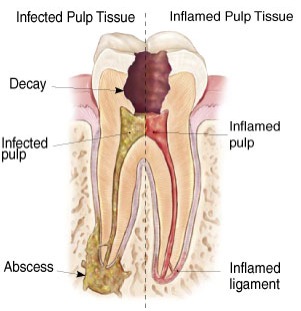 Endodontic treatment is necessary when the pulp or soft tissue inside of the tooth becomes infected and/or inflamed due to a variety of causes: deep decay, repeated dental procedures on the tooth or a crack or chip in the tooth. Even if the tooth has no visible chips or cracks, the tooth can have damaged pulp and when left untreated, it can cause pain or lead to an infection (abscess).
Endodontic treatment is necessary when the pulp or soft tissue inside of the tooth becomes infected and/or inflamed due to a variety of causes: deep decay, repeated dental procedures on the tooth or a crack or chip in the tooth. Even if the tooth has no visible chips or cracks, the tooth can have damaged pulp and when left untreated, it can cause pain or lead to an infection (abscess).
The pulp extends from the crown of the tooth to the tip of the roots and assists in a tooth’s growth and development. Once fully matured, however, the pulp is no longer essential to the tooth’s survival.
When the living tissue inside of the tooth is infected, an Endodontist must remove the pulp and clean the root canals completely before stabilizing the tooth structure.
After the canals are carefully cleaned and shaped, the canals are then filled with a rubber-like material called “gutta-percha.” The gutta-percha is placed with an adhesive cement to ensure complete sealing of the root canals.
Once the canals are completely restored, a temporary filling is placed by the Endodontist to close the opening before the tooth is restored by your general dentist. Since the tooth’s structure has been compromised during the treatment, the tooth must be properly restored by your general dentist as soon as possible.
Who Performs Root Canal Procedures?
“Endodontists” are dentists with at least two additional years of advanced training in diagnosis and treatment of root canal procedures. Upon graduation from dental school, Endodontists undergo extensive training to become specialists in the field.
As they are specialists in the field, Endodontists limit their practices to root canal treatments, and perform these services routinely. They also employ their expertise in treating difficult cases, such as teeth with narrow or blocked canals, or unusual anatomy.
Endodontists use advanced technology, such as operating microscope, digital imaging, and ultrasonic devices to perform these procedures.
Signs and Symptoms
• Prolonged sensitivity to hot and/or cold
• Tenderness to touch and chewing
• An abscess (often a pimple-like bump) on the gum tissue
• Swelling and/or drainage
• Persistent shooting/throbbing pains in the tooth
• Discoloration of the tooth structure
Often, however, there may be no symptoms.